Bursitis Treatment with LLLT/PBMT
Low-Level Laser Therapy (LLLT), also known as Photobiomodulation Therapy (PBMT), involves the application of red and near-infrared light to injuries to stimulate cellular repair. Led by Dr. Shikha Parmar, a GP with expertise in the management of chronic musculoskeletal pain, Laser Pain Therapy incorporates LLLT as part of a holistic treatment plan. LLLT is a highly effective, painless, and completely safe treatment in Melbourne, Victoria. LLLT treats the underlying cause of the injury, helping to reduce inflammation and support tissue regeneration. Supported by scientific research from respected institutions such as Harvard University and NASA, LLLT is an evidence-based therapy for bursitis.
Gentle. Drug-Free. Clinically Proven
Key Points
- Bursitis is the inflammation of a bursa, a fluid-filled sac that cushions joints and reduces friction between tendons and bones.
- In many cases, bursitis is secondary to underlying mechanical overload, tendon dysfunction, or adjacent soft tissue injury.
- The bursa sits between tendons, muscles, and bones to reduce friction. If the tendon is overloaded, degenerative, or mechanically impaired, altered biomechanics lead to increased friction, compression, or shear forces across the bursa, causing reactive inflammation and clinical bursitis.
- Common causes include repetitive movements, overuse, trauma, and age-related degeneration.
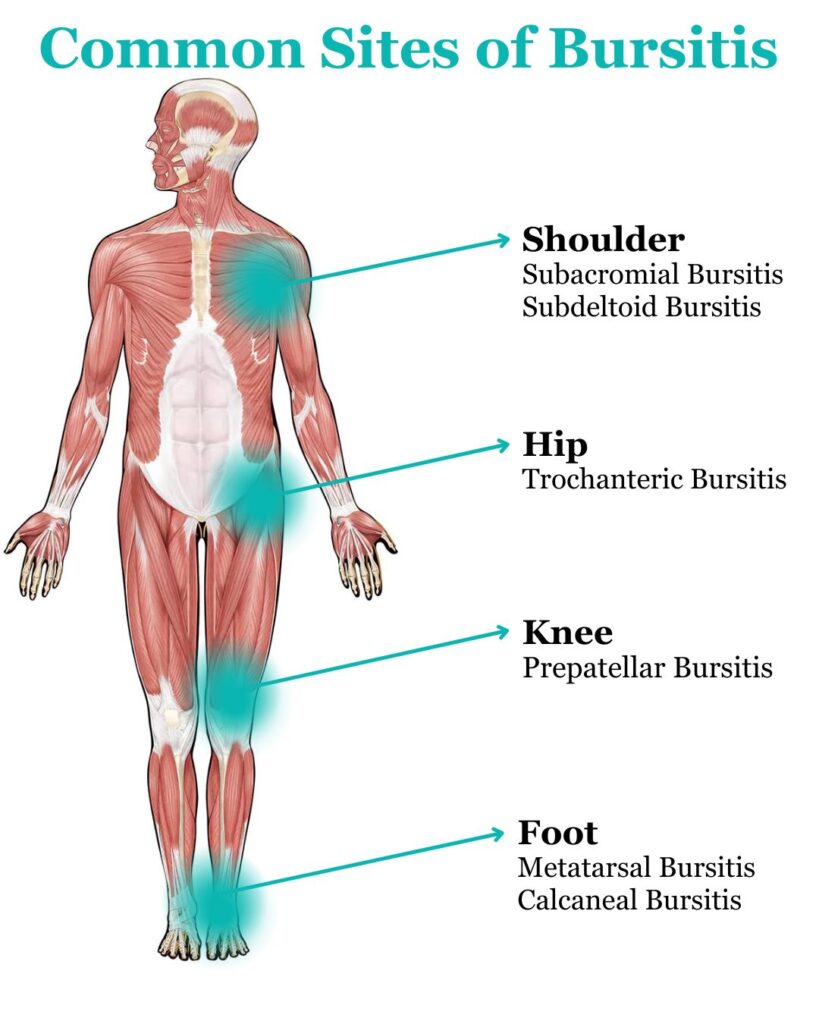
- Common sites affected by bursitis include the shoulder, elbow, knee, hip, and heel.
- LLLT can be highly effective in treating deep forms of bursitis, reducing inflammation, and promoting tissue repair.
- LLLT is not suitable for bursitis involving visible, localised swelling (e.g., in the knee or elbow) due to fluid buildup; draining may be necessary first.
- LLLT is a non-invasive, drug-free treatment that aids in healing and restores function, enabling rehabilitation and strength training.
What is Bursitis?
Bursitis is the inflammation of a bursa, a small, fluid-filled sac that acts as a cushion between bones and soft tissues, such as muscles, tendons, and skin. Bursae reduce friction and allow smooth movement of these structures. When a bursa becomes inflamed, it can cause pain, swelling, and limited movement. Bursitis commonly occurs in joints such as the shoulder, elbow, knee, and hip, often as a result of overuse or trauma. Chronic bursitis can lead to long-term discomfort and impaired mobility if not treated effectively.
Causes of Bursitis
Several factors contribute to the development of bursitis:
- Repetitive Movements: Continuous motion or pressure on a joint can irritate the bursa, causing inflammation. Activities such as kneeling, lifting, or overhead movements can strain the bursa.
- Overuse: Excessive use of a joint without adequate rest or recovery increases the likelihood of bursitis, especially in athletes or individuals who perform repetitive tasks.
- Trauma or Injury: Direct blows or falls onto a joint can irritate or damage the bursa, leading to inflammation.
- Age-Related Changes: As we age, the bursae become less resilient, making them more susceptible to inflammation.
- Infection: In some cases, bursitis can be caused by an infection, leading to more severe symptoms and requiring immediate medical treatment.
Common Sites Involved
Bursitis can occur in several areas of the body, including:
- Shoulder: The subacromial bursa in the shoulder is commonly affected, especially in individuals performing overhead activities. Read more here.
- Hip: Trochanteric bursitis, affecting the hip, is common in runners or those who frequently engage in side-to-side movements. Read more here.
- Knee: Various bursae of the knee can become inflamed from activities such as kneeling. Read more here.
- Foot: The bursa located at the bottom of the foot, often near the base of the big toe (Bunion bursitis) or in the heel (retrocalcaneal bursitis), can become inflamed, usually due to pressure from poorly fitted footwear or repetitive stress, such as walking or running. Read more here.
- Heel: The bursa between the heel and the Achilles tendon can become inflamed, often due to excessive pressure from activities such as running. Read more here.
In Many Cases, Bursitis is Secondary to Underlying Tendon Dysfunction
In many cases of bursitis, especially outside purely traumatic or infective causes, the condition is often secondary to underlying mechanical overload, tendon dysfunction, or adjacent soft tissue injury. The bursa acts as a friction-reducing structure between tendons, muscles, and bones. When the underlying tendon is overloaded, degenerated, or mechanically impaired, altered biomechanics cause increased friction, compression, or shear forces across the bursa, which leads to reactive inflammation, resulting in clinical bursitis.
Examples of Bursitis and Associated Tendon Involvement:
- Subacromial Bursitis: Associated with rotator cuff tendons (supraspinatus, infraspinatus, subscapularis).
- Trochanteric Bursitis: Often linked with gluteus medius/minimus tendinopathy.
- Pes Anserine Bursitis: Associated with overload of sartorius, gracilis, and semitendinosus tendons.
- Deep infrapatellar Bursitis: below the kneecap associated with patellar tendinopathy
A key distinction is that olecranon (elbow) bursitis and prepatellar knee bursitis – here tendon injury is not a common primary cause. In most other bursae, especially in chronic cases, bursitis is more likely to be reactive to altered tendon mechanics or muscle imbalance.
Symptoms
The symptoms of bursitis may vary depending on the location of the affected bursa but generally include:
- Pain: Localised pain over the affected joint, which may worsen with movement or pressure.
- Swelling: swelling around the affected area, often accompanied by warmth.
- Stiffness: A limited range of motion in the affected joint.
- Tenderness: Sensitivity when touching or applying pressure to the inflamed bursa.
- Reduced Function: Difficulty performing everyday activities due to pain or stiffness in the joint.
Diagnosis
Diagnosing bursitis involves:
- Medical History: Dr. Shikha Parmar will take a thorough history of symptoms, including any repetitive movements or activities that may have caused or exacerbated the condition.
- Physical Examination: A hands-on examination to assess pain, swelling, range of motion, and tenderness in the affected area.
- Imaging: X-rays or ultrasound may be used to confirm the diagnosis and rule out other conditions such as fractures or joint abnormalities. In some cases, MRI may be used to assess the extent of the inflammation or any tendon damage.
A Note About Superficial Visible Bursitis: For superficial bursitis that causes visible, localised swelling, such as in the knee or elbow (olecranon bursitis), LLLT/PBMT is not effective for treating significant fluid buildup. In these cases, draining the bursa may be necessary before further treatment. However, LLLT is very effective for deeper bursitis forms, often associated with tendon or ligament injury, osteoarthritis, degenerative conditions, or cartilage damage. By reducing inflammation and promoting tissue repair, LLLT helps manage pain and restore function, enabling rehabilitation and strength training.
Treatment Using LLLT/PBMPT
Why Choose Low Level Laser Therapy (LLLT)?
Many patients come to us after trying various other approaches with only limited or temporary relief. LLLT offers a scientifically validated, gentle, and highly effective treatment option. By addressing the root cause of bursitis, it promotes true healing from the inside out without side effects. LLLT restores balance to the inflammatory process, supports tissue healing, and reduces pain.
Common, conventional approaches such as icing, stretching, exercises, massage, or anti-inflammatory medications may temporarily ease symptoms but do not target the underlying problem. In some cases, these approaches can even aggravate sensitive or damaged tissues, including exercise introduced too early.
- Ice: Beyond the first 24 hours, ice can impede healing by reducing blood flow. Read more here.
- Anti-inflammatories: While they can reduce inflammation temporarily, they may delay natural healing and cause side effects when overused.
- Cortisone (or steroid) injections: May provide short-term relief but do not promote tissue repair and can weaken tendons, leading to recurrence.
- PRP injections: These are invasive, painful, and only offer limited effects in specific areas. Evidence for their efficacy remains inconsistent.
Splints: In some cases, splints may be used to support and stabilise the affected joint, reducing stress on the injured area during daily activities. Splints help keep the joint in alignment and limit movement, providing relief from strain. Additionally, splints may be recommended during the initial resting phase to allow the bursa to heal and prevent further irritation. This can be especially useful in the early stages of bursitis to promote recovery.
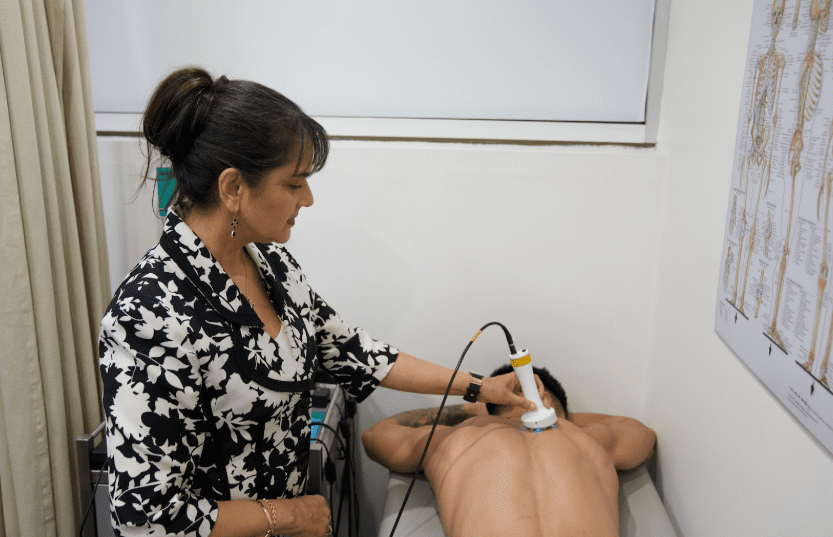
At Laser Pain Therapy, we use Low Level Laser Therapy (LLLT) as a core component of a holistic, medically supervised six-week treatment program, including rehabilitation support tailored to each patient’s specific needs. Led by Dr. Shikha Parmar, a GP with a special interest in musculoskeletal injury and pain, our clinic provides safe, non-invasive, and evidence-based care under direct medical supervision.
LLLT is ideal for bursitis where inflammation and micro-trauma persist, and where mechanical stress must be avoided during recovery.
How LLLT Works
Inflammation is the body’s natural response to injury, essential for initiating healing. However, when this response becomes chronic or excessive, it can disrupt the body’s own repair mechanisms, resulting in prolonged pain and dysfunction. LLLT addresses this imbalance by restoring proper immune function and creating optimal conditions for tissue regeneration.
Read how LLLT does this here.
LLLT uses red and near-infrared light to promote healing and tissue repair at the cellular level. Through scientific and clinical studies, LLLT has been shown to:
- Improve blood flow and oxygen delivery to tissues, promoting healing.
- Enhance lymphatic drainage and waste removal, supporting the detoxification process.
- Reduce inflammation by addressing oxidative stress, a major cause of many musculoskeletal conditions.
- Stimulate cellular energy (ATP) production, which accelerates tissue repair.
- Support tissue regeneration, helping restore balance to the immune response.
Importantly, LLLT does all of this without applying mechanical stress to the injured area, facilitating true healing without aggravating the injury.
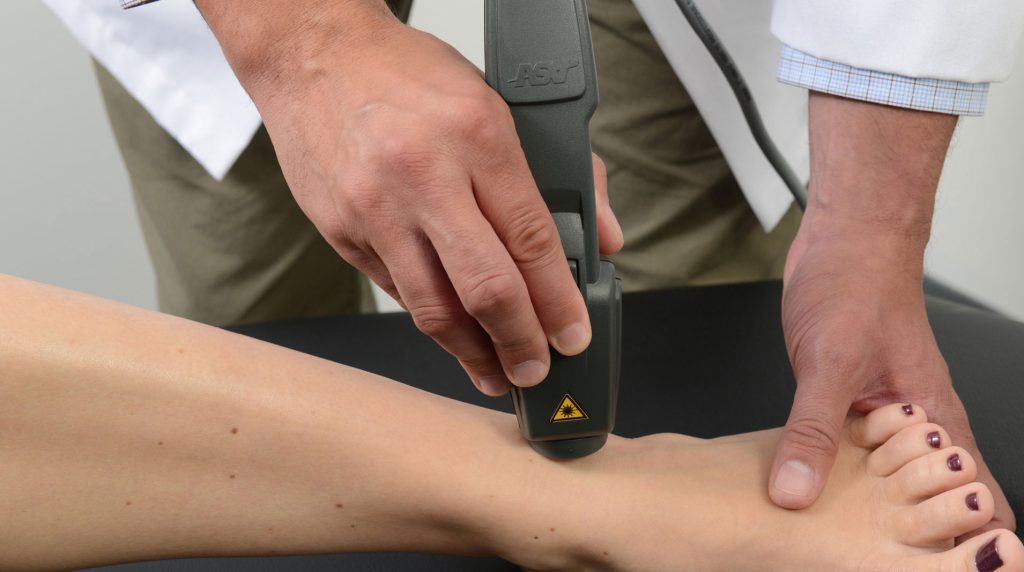
Proven, Safe, and Effective
LLLT/PBM Therapy is supported by more than 700 randomised controlled trials and over 7,000 studies. It is used worldwide in thousands of clinics, hospitals, and elite sports institutions.
LLLT/PBMT offers numerous benefits:
- Scientifically proven and evidence-based
- Non-invasive, painless, and drug-free
- No effect on normal tissues, safe, and non-toxic, with no side effects
- Clinically proven to eliminate pain, promote natural healing and tissue regeneration, and restore function
- Provides long-term relief, addressing the root cause of musculoskeletal pain
At our GP-led clinic, we combine expert medical assessment with the latest non-invasive therapies. Every patient is seen by Dr. Shikha Parmar to ensure accurate diagnosis and management planning. Treatment delivery is performed by highly trained assistants under direct medical supervision.
Clinical Outcome Goals
Treatment at Laser Pain Therapy is finite and aims to:
- Relieve pain and reduce inflammation
- Promote healing of the affected bursa
- Improve strength, stability, flexibility, and overall function of the affected area
- Safely rebuild strength through progressive rehabilitation as symptoms subside to support sustainable return to normal activity
Continuing LLLT during rehabilitation aims to enhance tissue quality, leading to stronger, more resilient tissues and superior long-term recovery outcomes compared to conventional methods.
Treatment Plan
Our Low Level Laser Therapy (LLLT) program is structured, time-limited, and medically supervised by Dr. Shikha Parmar. Each patient receives a comprehensive assessment that takes into account their health history, medications, lifestyle, work, personal activity demands, and any nutritional deficiencies. This holistic approach allows us to tailor the care plan with LLLT at the core, supported by personalised advice.
Our standard treatment program includes:
- Up to 12 LLLT sessions, with a review after 6 to assess early progress
- Individualised advice for managing the injury and activity modification
- A guided rehabilitation and return-to-function plan to support long-term recovery
While outcomes vary, we typically expect a 15–20% improvement in pain or function within the first 6 sessions if the treatment is likely to be effective. If this threshold isn’t met – which is uncommon – we will reassess the treatment plan, and treatment is generally not continued. The number of sessions can be adjusted based on progress and discussed in detail with the patient.
If there is a treatment response after the 2 to 3 weeks, we recommend 6 further treatments, along with introducing our protocol of light and gradual graded rehab, to effect a path to resolution of perhaps up to 70 to 90% improvement in best case scenario. Ongoing treatment beyond an anticipated 12-treatment protocol is not required, as your own immune system will continue the healing process once laser therapy is withdrawn.
All treatment decisions are made collaboratively, keeping the patient’s progress, preferences, and medical context in mind.
Ready for Lasting Relief?
If you are struggling with knee bursitis or related soft tissue injuries, we invite you to contact our experienced team at Laser Pain Therapy. Our LLLT treatment offers a safe, effective, and lasting solution to restore your comfort, mobility, and quality of life.
Contact us today to arrange your consultation and take the first step towards recovery.
📍 Located in Melbourne
📞 (03) 8529 2225 Contact Us